Back in 2009, what would become the Howard University Health Sciences Simulation and Clinical Skills Center, had just a single phone line, a $100,000 operating budget and the vision of its founders to provide “a multidisciplinary facility to support the interprofessional education and skills development across the health sciences.”
Today, as Howard celebrates the 15-year anniversary of the center’s first phase (the clinical skills center) and the 10-year anniversary of the second phase (the simulation center), that vision has come to fruition with a $3.5 million annual budget, five different managers, and eight full-time staff people; who annually train 800 to 900 future physicians, dentists, nurses, pharmacists, and other health care professionals to become the world-class leaders of tomorrow.

Over the years, the $8 million center has also become world-renowned for its state-of-the-art technology, the quality of its teachers, and how it has expanded the use of simulation to promote interprofessional education and patient safety. It is one of the few such centers to be accredited by the American College of Surgeons, an honor it’s held since 2016.
“There are many, many, many simulation centers in this world, but to obtain accreditation means that we have met a standard that is sought after by many other centers so we’re very proud of that,” said Debra Ford, MD, the center’s founding medical/surgical director and senior associate dean for academic affairs.
Though it was developed for the health sciences schools, it now provides services to 12 of the 14 schools and colleges across campus as well as the community, such as DC Fire and EMS. What’s more, the center has become so well-respected, schools such as Georgetown University regularly use it to train its own students. It’s become a must-stop for world leaders and heads of state visiting Howard, including numerous African leaders and President Barrack Obama.
When I came here there was an interest and a hunger, but I didn’t know how much it would catch fire.”
“It’s really surreal looking back on it all,” said Tamara Owens, PhD, founding director for the Simulation and Critical Skills Center and an internationally known expert in standardized patient education and simulation who was recruited in 2009 by then Dean of College of Medicine, Robert Taylor, MD. “When I came here there was an interest and a hunger, but I didn’t know how much it would catch fire.”
The center especially appeals to students, who learn vital clinical and technical skills in a controlled setting, Ford said. “We wanted to build a center that focused on Interprofessional Education (IPE). One of the important aspects of IPE is teaching all health care learners how to communicate with each other, how to understand what everyone does and what their role is in taking care of the patient. Simulation is built for that,” she said.
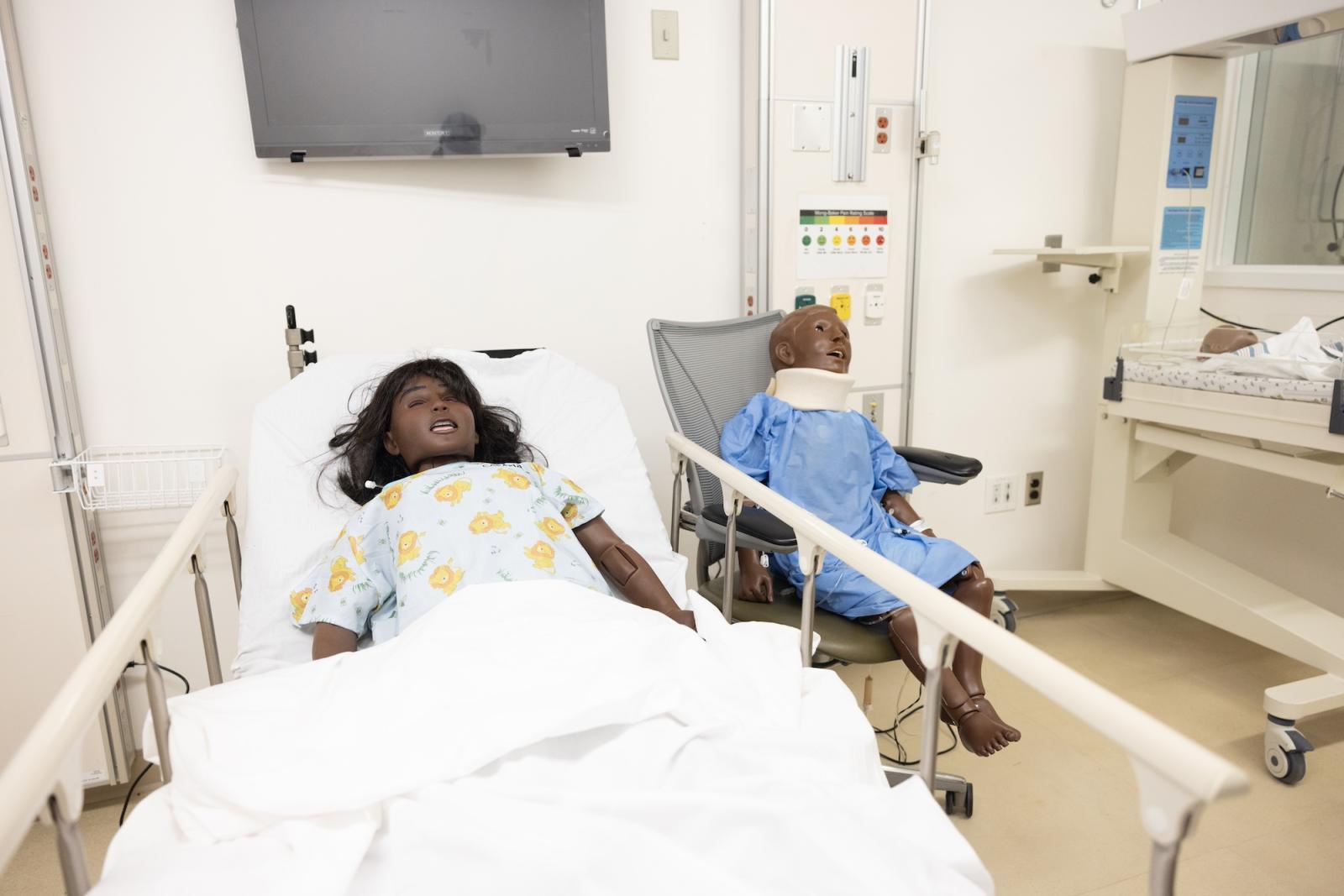
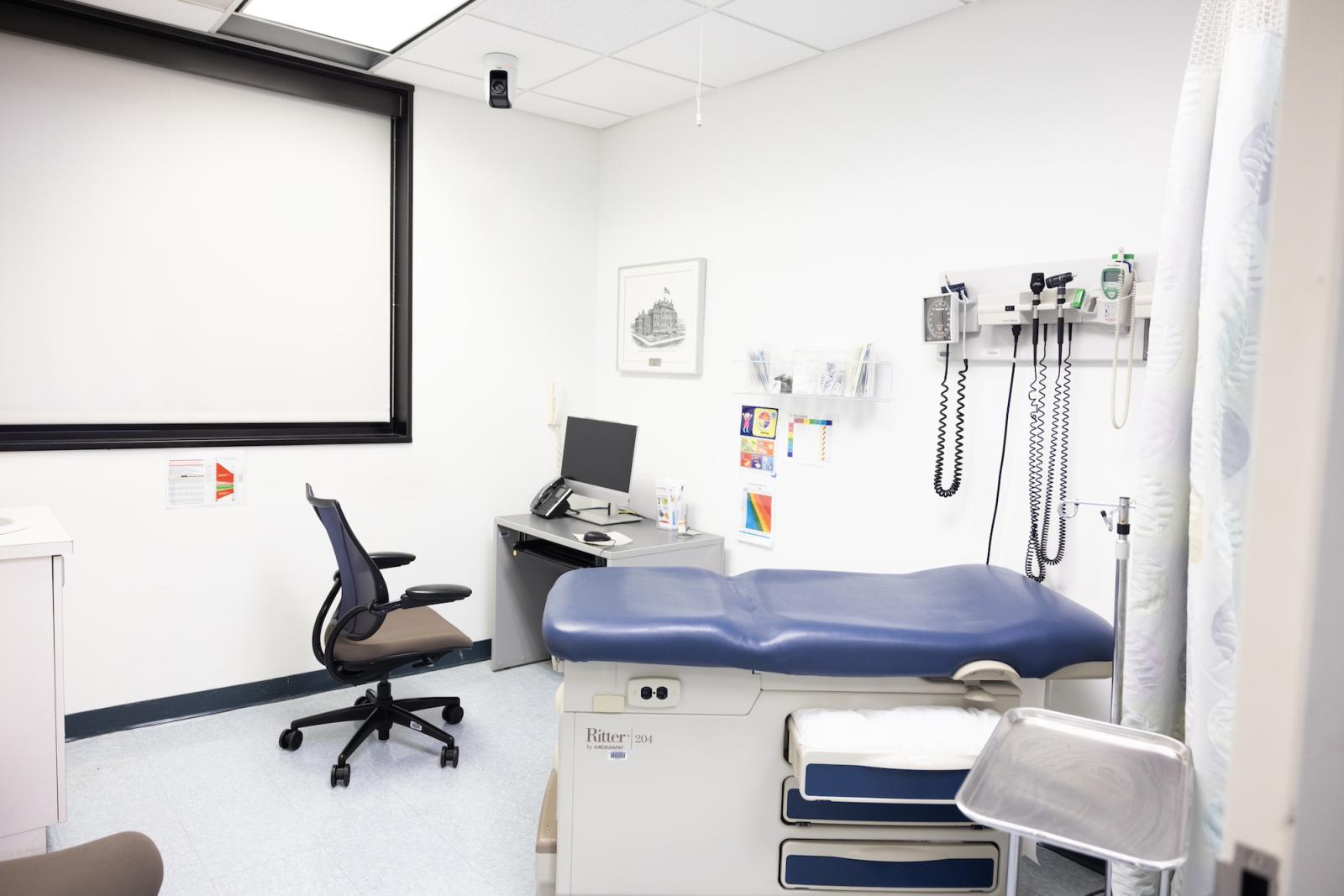
Just as the name implies, the Simulation and Clinical Skills Center uses a variety of technology and trainers to simulate real-world medical conditions — including mannequins, virtual reality trainers, human simulators, mock OR, and delivery suite. Through these simulations, Ford said students learn a number of key skills including how to obtain patient histories, conduct physical examinations, learn bedside procedures, ultrasound, and neonatal resuscitation.
Because this is a Howard center, all of the training is done with diversity, inclusion and equity in mind. For example, mannequins come in all skin tones and students regularly consider the underserved patient. “When we give verbal feedback, we’re always talking about whether the patient might not have enough money or food,” Owens said. “We are always thinking from a lens of health justice. But many of my colleagues in the field don’t think that way.”
That’s why so many institutions have turned to Howard over the years to bring more diversity, equity and inclusion into their programs. “We don’t think about that here, because we’re always inclusive,” Owens added.
Going forward, that inclusivity will grow into more research as the center moves into the planned Health Sciences Complex expected to be completed by 2027. That complex will include 30,000 square feet for an expanded Simulation and Critical Skills Center — more than twice its current 12,000 square feet.
“We need research for those that look like us,” Owens said. “And we need Black and brown people doing that research and sharing the findings.”

In addition to research, Owens and Ford said the new complex will allow simulation and critical skills — currently physically separated — to exist on a single floor. As with the center’s vision over the past 15 years, the expanded center will continue focusing on cutting edge technology designed to prepare students for what’s next. For example, 3D rooms are envisioned that simulate real operating rooms with a more immersive experience.
“We’re thinking about how to bring AI and virtual reality and all the latest in simulation into this new space so we can help our learners be ready for what’s current — and what’s coming in the future,” Owens said.
Article ID: 1911




